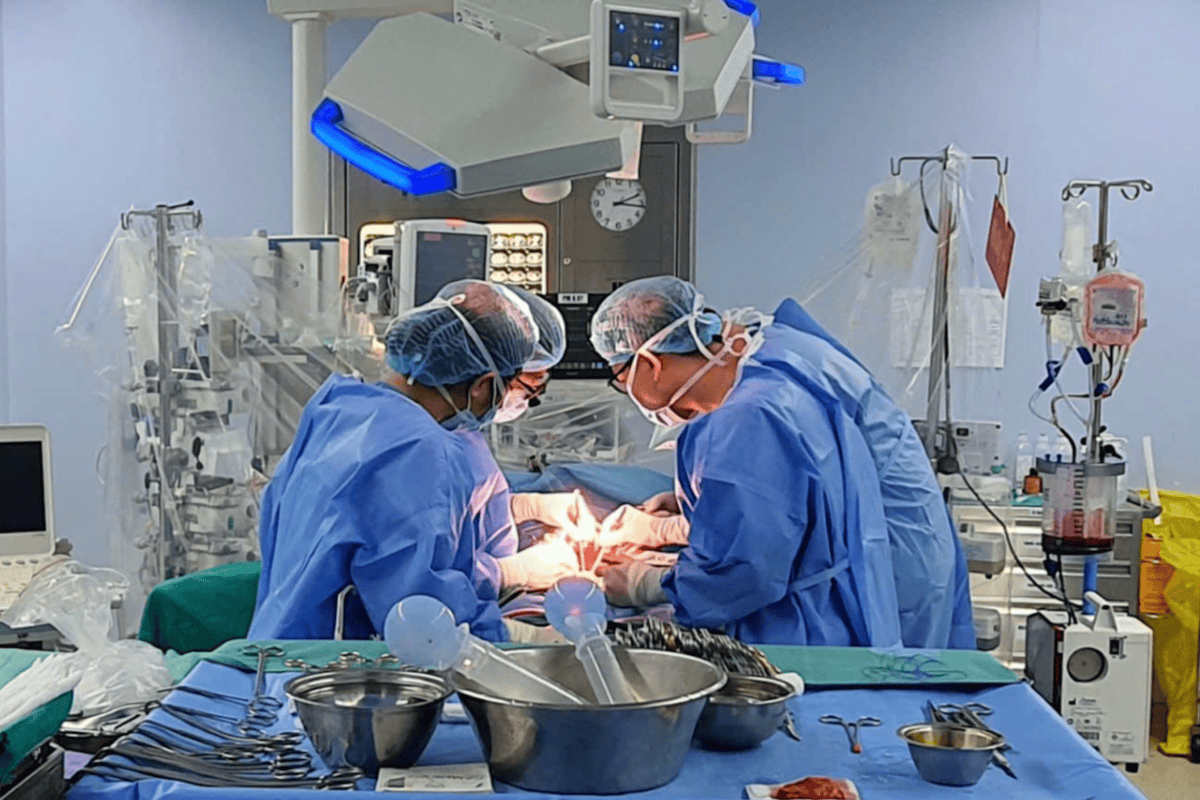
February 2025 marks the two-year anniversary of H bravely donating a part of her liver to her brother. After the liver transplant surgery, she has returned to her daily teaching work in healthy physical conditions. K, her brother, has also come back to his normal life, working in the transport services sector.
In late 2022, while working in South Korea, K. showed symptoms of acute liver failure from chronic liver disease due to hepatitis B. He was hospitalized and treated at a local hospital, but his condition did not improve, and the costs were high. Therefore, he decided to return to Vietnam to seek a chance to live.
As his condition worsened, doctors said the patient needed a liver transplant which was considered the optimal option, and the last hope to save the patient.
K. was transferred to the Central Military Hospital 108 in a critical condition: grade I-II hepatic encephalopathy, a severe liver function disorder. He was at risk of hepatic coma, and close to death.
His wife was ready to donate her liver to save him. However, her liver anatomical indices were not suitable, and surgery could pose high risks to both donor and recipient.
When all hope seemed exhausted, K.'s sister, a teacher in Nghe An, traveled 300 kilometers to the hospital, vowing to save her younger brother. The emergency liver transplant consultation was quickly carried out. An emergency liver transplant indication was issued and started early in the evening.
The surgery lasted seven hours until 3am. Since the patient had prolonged liver failure accompanied by serious blood clotting function disorders, the surgery faced significant challenges.
Removing the diseased liver was difficult due to liver cirrhosis, which made the liver tissue very prone to bleeding. The surgeons needed to be very careful to minimize the risk of damaging small blood vessels. Hemostasis became the biggest challenge, as significant blood loss could worsen the patient’s complications.
After removing the diseased liver, the doctors entered a tense strategic battle: performing the vascular and bile duct anastomoses to transplant the right liver lobe from the donor to the recipient. This was the critical phase for the success of the transplant, requiring meticulous attention to every detail.
"The anastomoses are very small, requiring absolute precision, almost no opportunity for correction. Just one misaligned suture could have led to bleeding or the formation of blood clots, posing serious post-operative complications," said Nguyen Hoang Ngoc Anh from the Department of Hepatobiliary and Pancreatic Surgery, Central Military Hospital 108.
Thao Trinh